Diffuse Large B-Cell Lymphoma Beyond the Nodes: A Case Series of Rare Extranodal Presentations in the Nasopharynx, Breast and Central Nervous System
Download
Abstract
Background: Lymphomas may originate from nodal or extranodal sites, with an increasing proportion of patients presenting with extranodal non-Hodgkin Lymphoma (NHL). Diffuse large B-cell lymphoma (DLBCL) is the most common subtype of NHL, seldom involves the nasopharynx, breast or central nervous system (CNS).
Objectives: In this study we described three rare primary extranodal presentations of DLBCL.
Methods: One case was nasopharyngeal DLBCL in a 13 years old boy who presented with recurrent nasal bleeding, obstruction, and discharge. Second case was breast DLBCL in a 72 years old female patient who had chief complaint of right breast lump for last 1 month without axillary lymphadenopathies. We had third case of DLBCL involving brain in a 50 years old male patient who had persistent headache and dizziness.
Case presentation: All the three cases had clinical suspicion of malignancy which was most common in that site.
Conclusion: Hence these cases emphasized the diagnostic importance of histopathology and immunohistochemistry in arriving at the correct diagnosis.
Introduction
Lymphomas represent a diverse group of malignant neoplasms derived from lymphocytes, characterized by clonal proliferation of these cells or their precursors due to somatic mutations [1]. They are broadly divided into Hodgkin lymphoma (HL) and non-Hodgkin lymphoma (NHL), which differ in morphology, immunophenotype, biology, and clinical presentation. NHL is further subclassified into B- and T-cell types, with precursor and mature B-cell categories recognized within the B-cell group. Among them, Diffuse Large B-cell Lymphoma (DLBCL) is the most frequently diagnosed NHL worldwide. Based on gene expression profiling (GEP), DLBCL can be categorized into germinal center B-cell (GCB)-like, activated B-cell (ABC)-like, and unclassifiable type 3 subgroups, each demonstrating distinct chromosomal alterations, signaling pathway activation, and prognostic differences [2]. Studies have shown that patients with the GCB subtype of DLBCL achieve higher complete response rates (~75-80%) with R-CHOP therapy compared to those with the ABC subtype (around 40-50%), reflecting the intrinsic molecular heterogeneity and prognostic differences between these subtypes [3, 4].
DLBCL is the most common primary B-cell neoplasm occurring in the head and neck region, with a predilection for the Waldeyer’s ring. Primary nasopharyngeal lymphoma is exceedingly rare, most often presenting as DLBCL or NK/T-cell lymphoma, with Epstein–Barr virus implicated in its pathogenesis [5].
It occurs more often in Asian populations and shows male predominance (55%) with a median age of 64 years. The disease typically presents in the sixth to eighth decades of life, although immunodeficiency may predispose to earlier onset [6].
Primary Breast Lymphomas (PBL) was first described in 1959 by Dobrotina [7]. It is uncommon entity which accounts for 0.1 - 0.15% of primary breast malignancies [8, 9]. Most primary breast lymphomas are of B-cell origin in which DLBCL is the most common diagnosis followed by MALT lymphoma, follicular lymphoma, Marginal Zone Lymphoma and Burkitt lymphoma [7, 10-12].
Primary central nervous system lymphoma (PCNSL) accounts for 3–4% of primary brain tumors and 4–6% of extranodal lymphomas, with a median diagnostic age of 65 years.
We are reporting three cases of primary extranodal DLBCL in rare sites. All patients were diagnosed as extranodal DLBCL variants (GCB, ABC or triple positive subtypes) via immunohistochemistry per the Hans algorithm.
Case 1
A 13-year-old boy presented to the ENT clinic with recurrent bilateral epistaxis and purulent nasal discharge for one month, followed by nasal obstruction, breathing difficulty, and sneezing for four days. There was no history of fever, facial pain, weight loss, night sweats or trauma. Examination revealed a posterior choanal mass without lymphadenopathy or organomegaly (Table 1).
| Case | Age | Gender | Site | Symptoms |
| 1 | 13 | M | Nasopharynx | Recurrent epistaxis |
| 2 | 72 | F | Right Breast | Breast lump |
| 3 | 50 | M | Posterior fossa Brain | Persistent headache |
Routine investigations were normal. On the basis of clinical examination, the initial differentials included adenoidal hypertrophy, lymphoproliferative disorder, and rhabdomyosarcoma. CT scan demonstrated a well-defined soft-tissue lesion arising from the posterior nasopharyngeal wall, extending into both choanae and compressing the right eustachian tube (Figure 1), with associated middle-ear effusion.
Figure 1. Non Contrast CT Scan Shows a Well Demarcated Iso-dense Mass in Nasopharynx (Arrow).
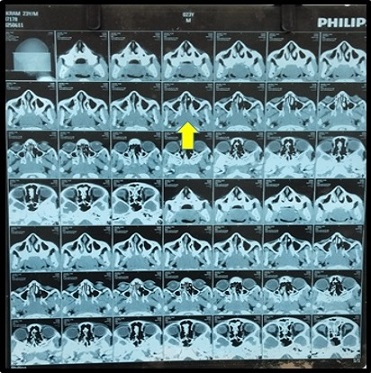
while 18F-FDG PET-CT showed a metabolically active nasopharyngeal lesion with FDG-avid (SUVmax~13.8) lymph nodes above and below the diaphragm, consistent with stage III disease and helped to exclude benign adenoid enlargement. The mass was excised surgically and sent for histopathology. Histopathology revealed diffuse infiltration by sheets of atypical medium- to large-sized lymphoid cells (Figure 2) displaying irregular round nuclei displaying moderate pleomorphism, vesicular chromatin, central prominent nucleoli and scant cytoplasm.
Figure 2. Microphotograph Displaying Fibrocollagenous Tissue Diffusely Infiltrating by Monomorphic Atypical Lymphoid Cell (100x; H and E).
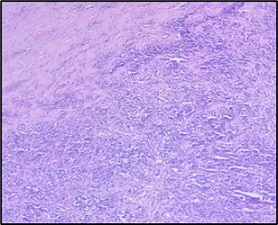
Frequent atypical mitotic figures and large area of necrosis also seen (Figure 3).
Figure 3. Microphotograph Displaying Sheets of Medium to Large Sized Atypical Lymphoid Cells Displaying Vesicular Chromatin and Central Prominent Nucleoli. Numerous atypical mitotic figures are also seen. (400x; H and E).
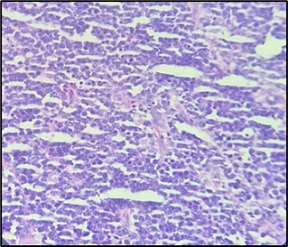
On suspecting malignancy, Immunohistochemistry was performed (Table 2) which leads to the diagnosis of DLBCL (GCB subtype) (Figure 4-6) and effectively excluded rhabdomyosarcoma.
| Case | Site | CD45 | CD20 | CD5 | CD3 | CD10 | CD79a | Bcl2 | Bcl6 | MUM1 | P53 | PD-L1 | Ki-67 |
| 1 | Nasopharynx | Positive | Negative | Positive | Negative | Positive | Positive | Positive | Positive | negative | Positive | Positive | 95% |
| 2 | Breast | Positive | Positive | Negative | Negative | Negative | Positive | Positive | Negative | Positive | *NA | *NA | 80-85% |
| 3 | Posterior Fossa Brain | Positive | Positive | Negative | Negative | Positive | Positive | Positive | Positive | Positive | *NA | *NA | 70% |
*NA, Not applied
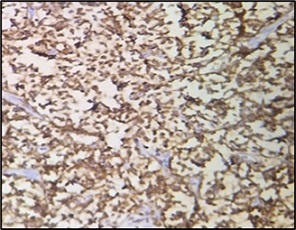
Figure 4. BCL6 Positive (400x; IHC).
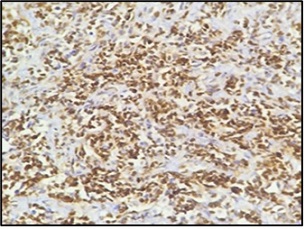
Figure 5. CD 10 Positive (400X; IHC).
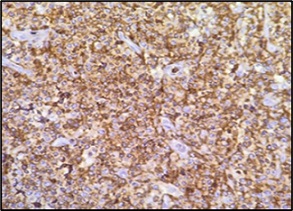
Figure 6. CD5 Positive (400X; IHC).
Due to CD20 negativity, standard anti-CD20 therapy alone was not feasible, and the patient was referred to a higher center for further management. The patient was initiated on a combination CHOP-based chemotherapy regimen including rituximab, hydrocortisone, cyclophosphamide, doxorubicin, vincristine and Mesna, along with supportive care to prevent toxicity and close monitoring of hematological and organ function. Unfortunately, the patient was lost to follow up, and the subsequent treatment response could not be assessed.
Case 2
A 72 years old female patient presented to Endocrine surgery OPD with a 1-month history of a right breast lump. On examination 5 x 3 cm swelling was seen in lower inner quadrant of right breast. It was firm, non tender with adjacent and overlying skin normal. Left breast was also normal. No axillary lymph nodes were palpable. On the basis of clinical examination, a suspicion of malignancy was made. Fine needle aspiration cytology was advised and it was suggestive of positive for malignancy, (Figure 7) and for further typing biopsy was advised We received Trucut biopsy of breast lump comprising of multiple grey white soft tissue cores collectively measuring 1.0 x 1.0 x 0.5 cm.
Figure 7. FNAC - Singly Scattered Tumour Cells Having Vesicular Chromatin and Prominent Nucleoli with Mitosis (arrow) (Giemsa 400X).
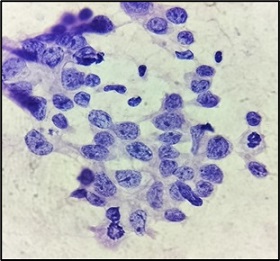
Microscopic features revealed fibro-collagenous tissue cores infiltrated by tumor cells which were predominantly scattered singly. These tumor cells were medium to large in size, having round to oval nuclei, irregular nuclear membrane, conspicuous nucleoli, vesicular chromatin and moderate amount of cytoplasm. Fair number of mitotic figures were noted (Figure 8).
Figure 8. Singly Scattered Atypical Lymphoid Cells. Mitotic figures are also evident. (H and E 400X).
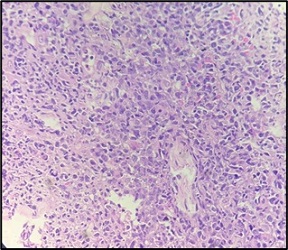
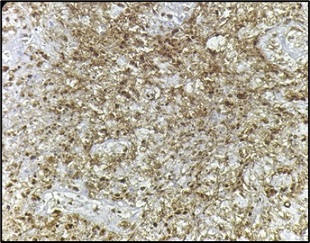
On the basis of histopathological features, differentials considered were metaplastic carcinoma and lymphoma. Immunohistochemistry was positive for CD45 (Figure 9), CD 19, CD20 (Figure 10), MUM-1 (Figure 11), BCL2 (Figure 12) and negative for ER, PR, Her2neu, P63, CK5/6, vimentin, CD3, CD5, CD10 and BCL6.
Figure 9. Tumor Cells are Diffuse and Strong Positive for CD45 (100X).
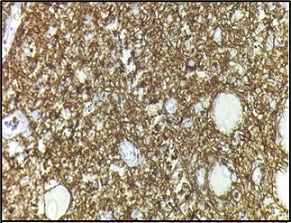
Figure 10. Tumor Cells Show Diffuse Cytoplasmic Positivity for CD20 (100X).
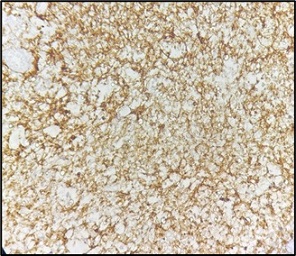
Figure 11. Tumor Cells Show Strong Positivity for MUM1 (100X).
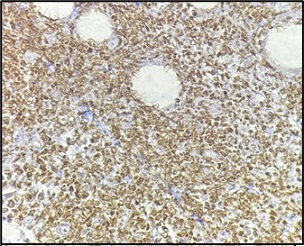
Figure 12. Tumor Cells Show Positivity for Bcl2 (100X).
While Ki-67 proliferative index was 80-85%. On the basis of histomorphology and IHC final diagnosis of DLBCL (Non Germinal Centre subtype) was made and effectively excluded metaplastic carcinoma. The patient was found to be non-metastatic on 18F-FDG PET-CT and a diagnosis of primary breast DLBCL, Stage IE was made. The case was discussed in a multi-disciplinary team meeting and the patient was started on R-CHOP regimen with rituximab, cyclophosphamide, doxorubicin, vincristine and prednisolone. Post 6 cycles of chemotherapy, the patient was found to have metabolic complete response on a repeat PET-CT and has been planned for Radiotherapy to the right breast. The patient has been advised strict follow up.
Case 3
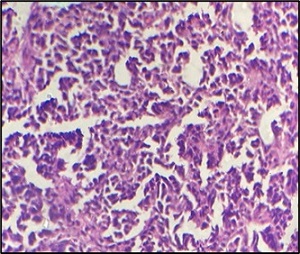
A 50-year-old male presented with six months of persistent headaches, dizziness, and fatigue, without neurological deficits or systemic illness. MRI brain revealed relatively well defined homogenously enhancing posterior fossa mass lesions suggestive of metastasis, high grade glioma or ependymoma. Surgical excision yielded firm, pearly-white tissue. The diagnosis of high- grade glioma was made on squash smear. Tumor tissue was further sent for histopathology. Microscopy showed brain parenchyma infiltrated by sheets of medium-to-large neoplastic lymphoid cells. No rosettes or fibrillary material was seen. The tumor cells were displaying hyperchromatic nuclei, inconspicuous nucleoli and scant cytoplasm. Frequent mitotic figures also seen (Figure 13).
Figure 13. Microphotograph Displaying Tumour Cells have Medium to Large Sized Hyperchromatic Nuclei with Inconspicuous Nucleoli and Scant Amount of Cytoplasm. Frequent mitotic figures are seen. (400x; H and E).
On the basis of histopathology, possibility of lymphoma was considered. Immunohistochemistry confirmed diffuse large B-cell lymphoma (DLBCL) (Table 2), triple positive for CD10, BCL-6, and MUM-1, with a Ki-67 index of 70% (Figure 14, 15).
Figure 14. CD10 Positive (400X; IHC).
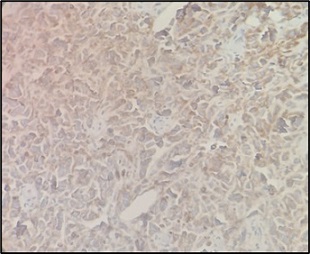
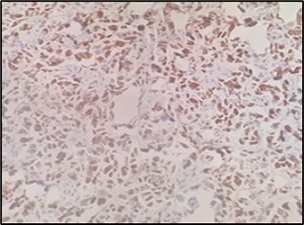
Figure 15. BCL6 Positive (400X; IHC).
The patient was discharged for adjuvant chemotherapy and advised to undergo six cycles of combination chemotherapy with rituximab, cyclophosphamide, doxorubicin, vincristine and prednisolone (R-CHOP regimen). He has completed one cycle of chemotherapy and is showing favourable clinical improvement. Supportive measures and close monitoring for hematological, hepatic and neurological toxicities was provided throughout the course of treatment. The patient continues remain under regular follow up for assessment of therapeutic response and completion of the remaining chemotherapy cycles.
Discussion
Primary DLBCL of nasopharynx
Diffuse large B-cell lymphoma (DLBCL) shows primary extranodal involvement in about 40% of cases, with a higher incidence in India (34–60%). Primary nasal cavity disease is rare (0.2–2%), though extranodal lymphomas of the tonsils, pharynx, and paranasal sinuses are usually B-cell derived. In India nasopharyngeal DLBCL is rare and may be influenced by region-specific factors such as Epstein-Barr virus (EBV) infection and underlying immunodeficiency, which can predispose to aggressive extranodal disease. A study by Rathaur et al. (1999) found that 70% of nasopharyngeal carcinomas in India were EBV positive with Type A EBV detected in 71.4% and type B in 25% of cases [13]. These factors contribute to the distinct biological behavior of nasopharyngeal lymphomas compared with conventional nodal DLBCL. Recognition of these influences is important for accurate diagnosis and appropriate therapeutic planning.
In our case patient had nasal bleeding, discharge, and obstruction without B symptoms. Because it mimics granulomatous or neoplastic conditions, timely recognition requires a high index of suspicion [14-16) Morphologically, it appeared as centroblastic. IHC typically shows positivity for CD45, B-cell markers (CD79a, CD19) and positivity for BCL2, BCL6 and CD10 with high Ki-67 index of 95%. This case is unique in view of its immunohistochemical profile, characterized by loss of CD 20 expression, aberrant CD5 positivity, P53 positivity and PD-L1 (5-10%) positivity, a combination that is rarely reported and complicates rituximab-based therapy.
CD5 expression is detected in approximately 5 to 10% of DLBCL cases and is often associated with aggressive clinical behavior [17]. Loss of CD20 expression is uncommon, observed in 1-2% of de novo DLBCL [18]. Overexpression of p53 occurs in about 20-40% of DLBCL and has been linked to poor prognosis [19]. PD-L1 expression in tumor cells is reported in approximately 5-10% of DLBCL cases, contributing to immune evasion mechanism [20]. So, early classification is crucial for managing DLBCL, with nasal cases treated similarly to other sites. Prognosis depends on stage and tumor burden, though sinonasal lymphomas often behave aggressively with relapse risk [21, 22]. A cohort study reported 56% overall survival and 50% five-year progression-free survival, with 22% recurrence in primary sinonasal DLBCL. Continuous surveillance and long-term follow- up are essential.
Primary DLBCL of Breast
Primary breast Lymphoma is rare entity. It typically a B cell origin which accounts for approximately 50% of all PBL [6, 23]. In general, patients give history of short duration with rapid increase in size. The clinical presentation is more or less similar to other breast carcinoma but single, painless palpable breast lump is the most common finding, however retraction of nipple and skin as well as nipple discharge are rarely seen. The usual B symptoms like fever, weight loss and night sweats which are seen in primary lymphoma are generally not seen in PBL [24, 25]. Some researchers mentioned that most frequent quadrant involved in decreasing order are upper outer, upper inner, lower outer and nipple/areolar region [25-27]. In the literature few authors described that association between lymphoma and pregnancy which suggest that hormonal disturbances play an important role in the pathogenesis of breast lymphoma [6]. PBL is mostly occur in females but few cases were reported in males also. Mean age at presentation is 60-65 years although it can also occur at younger age. Sakhri S et al [4] reported in the case series of PBL, one of their patients who is aged 17 years and associated with an aggressive prognosis.
Imaging features of PBL is nonspecific and may resemble with other breast malignancies. But very helpful in defining margin and vascularity of the lesion. PET CT play a crucial role in the evaluation of response to therapy and it is also valuable in the staging, metastasis and follow up [6, 28].
In DLBCL, Non- GCB type is commoner than GCB type. Wiseman and Liao [29] proposed the following three diagnostic criteria for PBL: (1) the mammary gland tissue and tumor tissue have a close relationship; (2) an appropriate histopathological evaluation has been performed; and (3) no malignant lymphoma is found at sites other than the mammary gland at the first visit, although ipsilateral axillary lymph node metastasis may be present. Our case met these criteria and was diagnosed as malignant lymphoma of the mammary gland. The histomophological features and IHC markers of our case are similar as described by Sakhri S et al [6], James ER et al [30] and Yoneyyama K et al [25].
James ER et al. [30] noted that Primary breast Diffuse Large B-cell Lymphoma (PB-DLBCL) necessitates systemic therapies, including chemotherapy, radiotherapy, and immunotherapy. The standard treatment regimen typically comprises six cycles of R-CHOP, which includes rituximab a monoclonal antibody targeting CD20 that depletes CD20-positive B cells along with a combination of four chemotherapeutic agents: cyclophosphamide, doxorubicin, vincristine, and prednisone. Sakhri S et al. [6] emphasized that treatment guidelines are contingent upon the histological subtype and clinical stage of the disease. It is well established that the CHOP regimen remains the standard therapeutic approach for primary diffuse large B-cell lymphoma (DLBCL) of the breast, with the recent incorporation of targeted therapies. Studies have shown that patients treated with R-CHOP achieve a 5-year overall survival rate ranging from 70% to 80%, reflecting significant improvement compared to historical outcomes with CHOP alone [31]. Polutazumab vedotin, an antibody-drug conjugate targeting CD79b on B cell, has emerged as a promising therapy for relapsed or refractory DLBCL. Although experience in primary breast DLBCL is limited [32].
Primary DLBCL of Posterior fossa of brain
Accounting for only 1–2% of non-Hodgkin lymphomas, primary CNS lymphoma is an infrequent but aggressive neoplasm. Diffuse Large B-cell lymphoma (DLBCL) constitutes the overwhelming majority of cases, with an incidence of approximately 84.6% [33, 34] Involvement of the central nervous system (CNS) is relatively rare in diffuse large B-cell lymphoma (DLBCL) when compared with other aggressive lymphomas, such as Burkitt’s lymphoma and lymphoblastic lymphoma [35] Symptomatology largely depends on the region affected and may include cranial neuropathies, prolonged headache, behavioral disturbances, changes in consciousness, and seizure activity [36, 37]. Radiological findings in CNS Lymphoma can vary significantly. Approximately 25% of patients may display atypical radiologic findings [38], which can complicate diagnosis of lymphoma, mimicking other conditions such as glioblastoma [39] or even neuroinflammatory diseases [40]. CNS relapses in DLBCL are rare but have devastating complications, occurring in 2–5 percent of overall cases [41]. In double expression lymphoma, the incidence of CNS relapse reaches 9.7 percent at 2 years [42].
The International Prognostic Index (IPI) is widely used to stratify risk and predict outcome in DLBCL, incorporating five parameters: age>60 years, performance status≥2, elevated serum lactate dehydrogenase (LDH), advanced stage (III-IV) and involvement of more than one extranodal site. Each factor scores one point, and the total score categorizes patients into low (0-1), low-intermediate (2), high-intermediate (3), and high risk (4-5) groups, correlating with overall survival [43].
The concurrent positivity for BCL6, CD10 and MUM- 1 observed in case no. 3, contrasts with the conventional immune-profiles reported in most DLBCL, highlighting its diagnostic complexity and rarity. These triple positive DLBCL are considered as heterogenous group and are enriched in IRF4 rearrangements. These rearrangements may drive B cell receptor signaling activation and contribute to aggressive disease biology. Such molecular features highlight the potential utility of targeted therapies, including Bruton’s tyrosine kinase (BTK inhibitors), particularly in relapsed or refractory cases, emphasizing the importance of integrating molecular profiling with conventional IHC to guide personalized treatment strategies.
In conclusion, this case series highlights the diagnostic complexity and clinicopathological diversity of DLBCL involving rare primary extranodal sites such as nasopharynx, breast and brain. Unusual immunophenotypic profiles underscores the biological heterogeneity of these cases. However, the small sample size and loss to follow up limit the generalizability and long-term prognostic interpretation of our findings. Despite these constraints, our observations add to the limited existing literature and emphasize the need for larger, multicentric studies with prolonged follow-up to better understand the behavior and therapeutic response of DLBCL at uncommon primary extranodal sites.
Declarations
Clinical trial registration
Not applicable
Conflicts of interest
Authors declare that they have no conflicts of interest.
Availability of data and material
The data sets used and/or analyzed during the current study are available from the corresponding authors per reasonable request.
Code availability
The custom code was used.
Originality Declaration for Figures
All figures included in this manuscript are original and have been created by the authors specifically for the purposes of this study. No previously published or copyrighted images have been used. The authors confirm that all graphical elements, illustrations, and visual materials were generated from the data obtained in the course of this research or designed uniquely for this manuscript.
Ethics approval
As per the norms of our university, ethical clearance is not required for publications based on case series, provided that patient identity is protected and informed consent has been obtained.
Consent to participate
Not applicable
Consent for publication
Informed/written consent was taken from all the three cases in the study for publication of their case.
Originality Declaration for Figures
All figures included in this manuscript are original and have been created by the authors specifically for the purposes of this study. No previously published or copyrighted images have been used. The authors confirm that all graphical elements, illustrations, and visual materials were generated from the data obtained in the course of this research or designed uniquely for this manuscript.
Acknowledgments
We extend our heartfelt gratitude to all the patients who generously contributed to this study. We are particularly thankful to technical and nursing staff of Department of Pathology, ENT, Endocrine Surgery and Neurosurgery, UPUMS, Saifai, Etawah.
Declaration on generative AI and AI-assisted technologies in the writing process
Not applicable.
References
- Clinicopathologic features and outcomes of diffuse large B-cell lymphoma with extranodal involvement: A retrospective analysis Nair SC , Gogia A, Arora S, Kumar L, Sharma A, Biswas A, Gupta R, Mallick S. Cancer Research, Statistics, and Treatment.2022;5(1). CrossRef
- Primary diffuse large B-cell lymphoma of the nasal bone and palate: An unusual clinical presentation Abeles EB , Umrau K, Gray ML , Boahene KD . Journal of oral and maxillofacial pathology: JOMFP.2022;26(4). CrossRef
- Molecular diagnosis of primary mediastinal B cell lymphoma identifies a clinically favorable subgroup of diffuse large B cell lymphoma related to Hodgkin lymphoma Rosenwald A, Wright G, Leroy K, Yu X, Gaulard P, Gascoyne RD , Chan WC , et al . The Journal of Experimental Medicine.2003;198(6). CrossRef
- Targeting B cell receptor signaling with ibrutinib in diffuse large B cell lymphoma Wilson WH , Young RM , Schmitz R, Yang Y, Pittaluga S, Wright G, Lih CJ , et al . Nature Medicine.2015;21(8). CrossRef
- Case Series of Rare Primary Intranasal Diffuse Large B-cell Lymphoma among Filipinos Cruz MV . Asian Pacific Journal of Cancer Care.. CrossRef
- Atypical Location of Diffuse Large B-cell Lymphoma in the Nasal Septum Patel V, Tacy CJ , Creamean T, Sibia A, Patel J. Cureus.2022;14(8). CrossRef
- Primary breast lymphoma: a case series and review of the literature Sakhri S, Aloui M, Bouhani M, Bouaziz H, Kamoun S, Slimene M, Ben Dhieb T. Journal of Medical Case Reports.2023;17(1). CrossRef
- Diagnostic surprise on IHC: A rare case of intramuscular DLBCL in thigh region mimicking sarcoma A. Ansari S, Agrawal T, Bhamra S. IP Archives of Cytology and Histopathology Research.2025;7(3). CrossRef
- Gaillard F. Breast lymphoma|Radiology Reference Article|Radiopaedia.org [Internet]. Radiopaedia. [cité 30 mars 2020]. Disponible sur: https:// radio paedia. org/ artic les/ breast- lymphoma Gailard F. .
- T-cell lymphoma presenting in the breast: a histologic, immunophenotypic and molecular genetic study of four cases Aguilera NS , Tavassoli FA , Chu WS , Abbondanzo SL . Modern Pathology: An Official Journal of the United States and Canadian Academy of Pathology, Inc.2000;13(6). CrossRef
- Primary breast lymphoma: 30 years of experience with diagnosis and treatment at a single medical center Radkani P, Joshi D, Paramo JC , Mesko TW . JAMA surgery.2014;149(1). CrossRef
- Three cases of malignant lymphoma of the breast Suzuki Y, Tokuda Y, Okumura A, Saito Y, Ohta M, Kubota M, Makuuchi H, et al . Japanese Journal of Clinical Oncology.2000;30(1). CrossRef
- Epstein-Barr virus in nasopharyngeal carcinoma in Indian patients Rathaur RG , Chitale AR , Banerjee K. Indian Journal of Cancer.1999;36(2-4).
- Fine needle aspiration cytology in lesions of the nose, nasal cavity and paranasal sinuses Gupta N, Kaur J, Srinivasan R, Das A, Mohindra S, Rajwanshi A, Nijhawan R. Acta Cytologica.2011;55(2). CrossRef
- Sinonasal B-cell lymphomas: A nationwide cohort study, with an emphasis on the prognosis and the recurrence pattern of primary diffuse large B-cell lymphoma Eriksen PRG , Clasen-Linde E, Nully Brown P, Haunstrup L, Christoffersen M, Asdahl P, Thomsen TM , et al . Hematological Oncology.2022;40(2). CrossRef
- Modern concepts in the biology, diagnosis, differential diagnosis and treatment of primary central nervous system lymphoma Deckert M, Engert A, Brück W, Ferreri AJM , Finke J, Illerhaus G, Klapper W, et al . Leukemia.2011;25(12). CrossRef
- CD5-positive diffuse large B-cell lymphoma: a retrospective study in 337 patients treated by chemotherapy with or without rituximab Miyazaki K, Yamaguchi M, Suzuki R, Kobayashi Y, Maeshima AM , Niitsu N, Ennishi D, et al . Annals of Oncology: Official Journal of the European Society for Medical Oncology.2011;22(7). CrossRef
- Age-related EBV-associated B-cell lymphoproliferative disorders: diagnostic approach to a newly recognized clinicopathological entity Shimoyama Y, Asano N, Kojima M, Morishima S, Yamamoto K, Oyama T, Kinoshita T, Nakamura S. Pathology International.2009;59(12). CrossRef
- Dysfunction of the TP53 tumor suppressor gene in lymphoid malignancies Xu-Monette ZY , Medeiros LJ , Li Y, Orlowski RZ , Andreeff M, Bueso-Ramos CE , Greiner TC , McDonnell TJ , Young KH . Blood.2012;119(16). CrossRef
- Expression of programmed cell death ligand 1 is associated with poor overall survival in patients with diffuse large B-cell lymphoma Kiyasu J, Miyoshi H, Hirata A, Arakawa F, Ichikawa A, Niino D, Sugita Y, et al . Blood.2015;126(19). CrossRef
- Epidemiologic Characteristics, Prognostic Factors, and Treatment Outcomes in Primary Central Nervous System Lymphoma: A SEER-Based Study Tang D, Chen Y, Shi Y, Tao H, Tao S, Zhang Q, Ding B, et al . Frontiers in Oncology.2022;12. CrossRef
- Influence of Rituximab on Central Nervous System Relapse in Diffuse Large B-Cell Lymphoma and Role of Prophylaxis--A Systematic Review of Prospective Studies Ghose A, Elias HK , Guha G, Yellu M, Kundu R, Latif T. Clinical Lymphoma, Myeloma & Leukemia.2015;15(8). CrossRef
- Primary breast lymphoma - a review of the literature and report of three cases Joks M, Myśliwiec K, Lewandowski K. Archives of medical science: AMS.2011;7(1). CrossRef
- Primary Breast Diffuse Large B-Cell Lymphoma in a 42-Year-Old Female: A Case Report and Review of Literature Chen M, Zhou J, Qu X. Journal of Medical Cases.2021;12(5). CrossRef
- Primary lymphoma of the breast: A case report and review of the literature Yoneyama K, Nakagawa M, Hara A. Radiology Case Reports.2021;16(1). CrossRef
- Primary lymphoma of the breast involving both axillae with bilateral breast carcinoma Garg NK , Bagul NB , Rubin G, Shah EF . World Journal of Surgical Oncology.2008;6. CrossRef
- Three Cases of Combined Therapy in Primary Breast Lymphoma (PBL) with Successful Outcomes Inic Z, Inic M, Zegarac M, Inic I, Pupic G. Clinical Medicine Insights. Oncology.2013;7. CrossRef
- Primary lymphoma of the breast: A case series Wadhwa A, Senebouttarath K. Radiology Case Reports.2018;13(4). CrossRef
- Primary lymphoma of the breast Wiseman C, Liao KT . Cancer.1972;29(6). CrossRef
- Primary Lymphomas of the Breast: A Review James ER , Miranda RN , Turner SD . JPRAS open.2022;32. CrossRef
- Primary diffuse large B-cell lymphoma of the breast: prognostic factors and outcomes of a study by the International Extranodal Lymphoma Study Group Ryan G, Martinelli G, Kuper-Hommel M, Tsang R, Pruneri G, Yuen K, Roos D, et al . Annals of Oncology: Official Journal of the European Society for Medical Oncology.2008;19(2). CrossRef
- Spotlight on polatuzumab vedotin: new standards for diffuse large B-cell lymphoma? Ghione P, Salles G. Haematologica.2024;109(9). CrossRef
- Central nervous system dissemination in immunocompetent patients with aggressive lymphomas: incidence, risk factors and therapeutic options Ferreri AJM , Assanelli A, Crocchiolo R, Ciceri F. Hematological Oncology.2009;27(2). CrossRef
- Secondary central nervous system lymphoma Tomita N, Kodama F, Kanamori H, Motomura S, Ishigatsubo Y. International Journal of Hematology.2006;84(2). CrossRef
- Primary lymphoma of the central nervous system: typical and atypical CT and MR imaging appearances Erdag N, Bhorade RM , Alberico RA , Yousuf N, Patel MR . AJR. American journal of roentgenology.2001;176(5). CrossRef
- Central nervous system lymphoma: characteristic findings on traditional and advanced imaging Haldorsen IS , Espeland A, Larsson EM . AJNR. American journal of neuroradiology.2011;32(6). CrossRef
- Primary central nervous system lymphoma in AIDS: a wider spectrum of CT and MRI findings Thurnher MM , Rieger A, Kleibl-Popov C, Settinek U, Henk C, Haberler C, Schindler E. Neuroradiology.2001;43(1). CrossRef
- Multiparametric MR Imaging Features of Primary CNS Lymphomas Talybov R, Beylerli O, Mochalov V, Prokopenko A, Ilyasova T, Trofimova T, Sufianov A, Guang Y. Frontiers in Surgery.2022;9. CrossRef
- Stand-alone intrathecal central nervous system (CNS) prophylaxis provide unclear benefit in reducing CNS relapse risk in elderly DLBCL patients treated with R-CHOP and is associated increased infection-related toxicity Eyre TA , Kirkwood AA , Wolf J, Hildyard C, Mercer C, Plaschkes H, Griffith J, et al . British Journal of Haematology.2019;187(2). CrossRef
- Impact of dual expression of MYC and BCL2 by immunohistochemistry on the risk of CNS relapse in DLBCL Savage KJ , Slack GW , Mottok A, Sehn LH , Villa D, Kansara R, Kridel R, et al . Blood.2016;127(18). CrossRef
- Differentiating glioblastoma from primary central nervous system lymphoma of atypical manifestation using multiparametric magnetic resonance imaging: A comparative study Feng A, Li L, Huang T, Li S, He N, Huang L, Zeng M, Lyu J. Heliyon.2023;9(4). CrossRef
- Lymphomas mimicking neuroinflammatory diseases - A diagnostic conundrum worth revisiting Raza SA , Raza M, Dai M, Husan A, Cotelingam J, AlHussein H. Journal of Neuroimmunology.2022;372. CrossRef
- The revised International Prognostic Index (R-IPI) is a better predictor of outcome than the standard IPI for patients with diffuse large B-cell lymphoma treated with R-CHOP Sehn LH , Berry B, Chhanabhai M, Fitzgerald C, Gill K, Hoskins P, Klasa R, et al . Blood.2007;109(5). CrossRef
License

This work is licensed under a Creative Commons Attribution-NonCommercial 4.0 International License.
Copyright
© Asian Pacific Journal of Cancer Care , 2026
Author Details
How to Cite
- Abstract viewed - 0 times
- PDF (FULL TEXT) downloaded - 0 times
- XML downloaded - 0 times